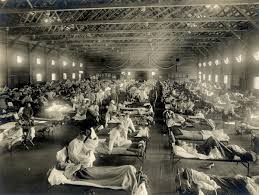
As we all try to acclimate ourselves to the rapidly changing circumstances brought about by the COVID-19 pandemic, comparisons are being made between this pandemic and the so-called Spanish flu pandemic of 1918-1919. (The reason it was referred to as the Spanishflu was that Spain was one of the only countries at the time to not censor reports of cases, and so it was widely publicized there by late-fall 1918.) The Spanish flu proved to be peculiar for several reasons, most noteworthy of course due to the high morbidity (as many 500 million were infected) and mortality (around 50 million deaths). It also came in waves. In the US, there were four such waves: first in spring 1918, again in August 1918 (epidemiologically the most devastating of the four), yet again in winter 1918/1919, and a final return in early 1920. Finally, the disease was unlike most flus in that it decimated even the traditionally more robust segments of the population (ages 20-40), taking the lives of many within 3 days of showing symptoms.
Exploring the pandemics
Since the pandemic of the Spanish flu, researchers dedicated themselves to identifying the origins and nature of the virus. It took decades, however, before virologists succeeded. Starting in the mid-1990s, Jeffrey Taubenberger, MD, PhD, and his team were able to carry out a sequence and phylogenetic analysis of 1918 influenza virus genes and identified it to be an H1N1 virus of avian origin.1
Until around 1970, historical research about the pandemic had been virtually non-existent. Some novels and popular histories appeared over the decades, but it was Alfred Crosby’s 1976 book Epidemic and Peace, 1918 (reissued in 1989 under the title America’s Forgotten Pandemic: The Influenza of 1918) that paved the way for international research about the subject.2 One of the book’s major achievements was to draw attention to the fact that the pandemic quickly disappeared as a topic of public conversation soon after it was over, ignored by periodicals and textbooks for decades. To many historians, this collective silence is as much a part of the pandemic’s story as the course of the disease itself.
The mental health links
In comparison to other aspects of the pandemic, little research has been done on the long-term impact of the Spanish flu on mental health. One of the few researchers to investigate the subject was historical demographer Svenn-Erik Mamelund, PhD. Looking at asylum hospitalizations in Norway from 1872 to 1929, Mamelund found that the number of first-time hospitalized patients with mental disorders attributed to influenza increased by an average annual factor of 7.2 in the 6 years following the pandemic.3 In addition, he pointed out that Spanish flu survivors reported sleep disturbances, depression, mental distraction, dizziness, and difficulties coping at work, and that influenza death rates in the United States during the years 1918-1920 significantly and positively related to suicide.4
Mamelund is among a number of scholars who have noted what many suspect to be a connection between the Spanish flu and a pronounced increase in neurological diseases. By 1919 and 1920, physicians and researchers in Great Britain were already reporting a marked rise in nervous symptoms and illnesses among some patients recovering from influenza infection; among other symptoms, depression, neuropathy, neurasthenia, meningitis, degenerative changes in nerve cells, and a decline in visual acuity were cited.5
Encephalitis lethargica: another connection or vulnerability?
Encephalitis lethargica coincided with the Spanish flu; it reached epidemic proportions alongside the Spanish flu. As Hoffman and Vilensky have recently described, the syndrome was characterized by two, often, blended phases:6
During the acute phase, patients typically experienced excessive sleepiness, disorders of ocular motility, fever, and movement disorders, although virtually any neurological sign or symptom could be exhibited, with day-to-day, and even hour-by-hour shifts in symptomatology. The chronic phase could occur months to years later and was most commonly characterized by parkinsonian-like signs.
Psychiatrists and neurologists first reported encountering encephalitis lethargica symptoms in 1916 and 1917 in Austria and France. By 1919, cases had become common throughout Europe, the United States, Canada, Central America, and India. All told, approximately 1 million people worldwide were affected by encephalitis lethargica between its outbreak in 1916 until the early 1930s. While many clinicians (both at the time and since then) have surmised an association between encephalitis lethargica and the Spanish flu,7 there is no conclusive evidence of causality.
Collateral damage
Some medical and social historians have been tracing connections between the pandemic and the other catastrophic global event of the time-World War I. In this regard, historians have flagged the ways in which the war efforts depleted medical personnel, helped disseminate the virus through the mobilization of troops, and created the conditions for the mutation of an otherwise mild flu virus.8
When it comes to mental health, the historical record shows that the pandemic, like the war, took a toll on the emotional resilience of those not (or not yet) in harm’s way. The massive and sudden loss of life plunged many into a chronic state of helplessness and anxiousness. A large portion of the population were affected by the loss of loved ones. Parents had to come to grips with losing a child (or even several children), while some children suddenly found themselves parentless. In November 1918, 31,000 children in New York City alone had lost one or both parents. For others, the experience left them feeling a mix of guilt, anger, confusion, and abandonment. Surviving health professionals were not immune to such sentiments, with many of them noting that they were haunted by a sense of frustration and grief, even years later.9
Like all mass encounters with infectious disease, the Spanish flu pandemic had its own unique features. If history teaches us anything, it is that we should always be measured in how we glean lessons from the past. That said, the example of the influenza of 1918-1920 gives us reason to expect that the present pandemic will carry in tow its own set of mental health challenges.
Source: Psychiatric Times