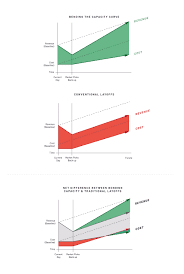
Political scientists emphasize the importance of “framing” in policy debates. The health care cost control debate in the United States has been reframed by the promotion of a metaphor, “bending the curve.” This metaphor has merits but they are decidedly mixed.
The sudden popularity of the idea of “bending the cost curve” is significant because it shows that, contrary to what policy specialists believe, politicians and interest groups do pay attention to the academic experts. Yet it is significant also because it frames cost control options in a way that favors some approaches at the expense of others, and some groups at the expense of others. In particular it reflects the dominance of the debate by budgetary perspectives, and favors the interests that benefit from high costs now by devaluing approaches that would reduce costs more quickly.
The Rapid Advent Of A Phrase
“Bending the curve” went from unfamiliar to “jargon” at warp speed. At the end of December, 2007, the Commonwealth Fund released a report on “Bending the Curve: Options for Achieving Savings and Improving Value in U.S. Health Spending.” Before that date, I can find, through journals’ own search engines, only one use of a similar phrase (e.g. “bend the cost curve” or “bending the cost curve”) in relation to U.S. health care in either of the two prominent health policy publications, Health Affairs or the New England Journal of Medicine. That was an interview with the Governor of Vermont in October of 2007. I find no use of similar terms in CQ Weekly, the closest thing to an authoritative source about Congress; and only one on the website of National Journal, the magazine and source of daily reports (such as Congress Daily and The Hotline) that is the main competition to CQ as an elite information source in Washington. I find no use in the New York Times from a search back to 1981.
By 2009, Health Affairs titled its September/October cost control issue “Bending the Cost Curve.” The term was ubiquitous in both experts’ and politicians’ commentaries. After skeptical testimony about the cost control effects of legislation by the Director of the Congressional Budget Office (CBO), Congressman Jim Cooper (D-Tennessee) blogged for National Journal that, “(i)n Washington jargon, he said the bills would bend the cost curves in the wrong direction.” (his emphasis) In an interview in February 2009, President Obama referred to the need for “bending the curve down on health care inflation,” not coincidentally in the context of “bending the [federal] deficit curve down.”
Karen Ignagni, CEO of the leading lobby for the health insurance industry, pledged in September 2009 that the industry would “do our part to bend the cost curve.” Senator Chuck Grassley (R-Iowa), senior Republican on the Finance Committee, in December blasted the bill under consideration in the Senate because it failed to “bend the cost curve the right way”. In perhaps the best indicator of a term’s use (or abuse), William Safire devoted one of his “On Language” columns in the New York Times to the “fast-blooming metaphor.”
Political Causes
Even if there were no substantive effects, the spread of this metaphor would reveal key aspects of health care politics. There could hardly be a better indication that expert discussions influence U.S. policy-makers. Moreover, it is a classic example of how health care policy and politics is often driven by budget politics.
What, a visitor from outer space or Europe might ask, is the “cost curve,” anyway? It is not the cost-benefit curve that would be familiar from discussions of “flat of the curve care.” That is a curve of diminishing returns – at some point more spending yields no benefit. The “cost curve” graphs spending over time, usually in units of constant dollars per capita, or share of GDP per capita. In any country this curve tends to slope upward; in the United States it slopes upward somewhat more steeply than in many countries, and from a higher base. It is a curve of increasing returns – to the health care sector, which gains an increasing share of the national economy.
“Bending” the curve means downward, to reduce the slope, so that spending will not be as high in the future as it would under current projections (in theory one could bend the slope negative, but that would not be “bending the curve,” it would be “cutting spending”). The message of this metaphor is about the future: that health care costs otherwise will at some point be “unsustainable,” so we must act now to prevent that from happening.
This raises a bit of a puzzle. One might expect that, with U.S. health care costs in 2008 sitting at 16 percent of GDP, and the next highest country just over 11 percent, politicians and business leaders and academics would have thought that the problem was that costs were too high at the time, rather than that they should be prevented from becoming too high in the future. Why, then, would anyone focus on the “cost curve,” rather than the costs?
One logical answer is that it’s a lot less threatening to the medical care establishment to talk about slowing cost growth in the future than about taking away some of their incomes now. One can have much more pleasant discussions, in which even the insurance companies will say they agree with the goal. Conflict is delayed or, more precisely, submerged. This pattern is reinforced by the policy choices usually associated with “bend the curve” rhetoric, as I discuss below. The Commonwealth Fund leadership surely did want to control costs, and sooner rather than later. But the term was picked up so widely, I suspect, in part because it is in many ways convenient to direct attention to the future rather than the present.
There is another reason the term was attractive: it fits with established patterns of both U.S. budgeting and crisis-mongering. Congressional budget procedures require that effects of legislation be estimated a decade into the future, and the CBO frequently reports on long-term deficit projections. The trustees of the Social Security and Medicare trust funds are also required to project balances far into the future. Therefore long-term projections of spending for health care programs, with graphs of potential trends, are an established part of the discussion.
But long-term projections have also become part of the political arsenal of the coalition of centrists and conservatives who, for different reasons, seek to raise fears about supposedly excessive federal spending. Throughout the budget battles of the 1980s and early 1990s, as the deficit did not do much immediate damage, budget hawks sought to scare others into action by extrapolating trends into a future when deficits might be enormously large, and so do economic damage. These arguments have focused on long-term projections of the costs of Social Security, Medicare and Medicaid, grouped as “entitlements,” with particular emphasis on the supposed crisis to come from an “aging society”. At present deficits actually are enormously large, but as a matter of economic necessity. So economists, as in a March 24, 2011 statement by 10 former chairs of the president’s Council of Economic Advisers, continue to emphasize the long-run: as in that group’s statement that, “repeated battles over the 2011 budget are taking attention from a more dire problem—the long-run budget deficit.”
Thus the health care “cost curve” fits easily into established thinking about long-term budget trends. President Obama’s connecting of the two topics is entirely normal in Washington, and the first use of a version of the term that I found was in the context of deficit-hawk politicians raising concern about the future in 2003: Republican Congresswoman Nancy Johnson saying that, “we have to bend the cost curve as the baby boomers retire”.
Analysts who focus on health care costs as a whole, or who believe social insurance programs are extremely important, have objected to this budgetary framing. They, including leaders of the Obama administration, have emphasized that the “budget” problem was really a “health care” problem. The problem is not the “entitlement” to care, but the system-wide increase in medical costs per capita.
From this perspective, the focus on budgetary costs of health care is particularly misguided in blaming the “entitlement” to medical care. We can see why by comparing the United States to other countries. The effects of aging on budgeted health care spending in the United States is particularly large in proportional terms not because the entitlement in the U.S. is excessive but because it is unusually limited. In the United States, for most people, on their 65th birthday, a large expense suddenly shifts to the federal government’s budget. In any other country, they remain in the same system they were in before. So the budgetary effect of aging in the United States is largely a cost shift, with corresponding savings to private budgets, rather than a cost increase. Moreover, the effect of population aging on government medical spending is particularly large in absolute terms in the United States because our baseline level of spending per person is already so much higher than in any other country.
For supporters of national health insurance and the Medicare program, the emphasis on the federal budget both overstates the societal effects of aging and diverts attention from most of the cost control challenge. Hence it seemed logical to meet the arguments about budgetary trends with arguments about system-wide medical spending trends. To do so, however, meant adopting the same frame about long-term “sustainability.”
Thus the “bending the curve” metaphor was picked up because it fits into the dominant discourse about a federal budget crisis, attracting conservatives and budget-focused elites; it is less threatening to the health care establishment than calls to “cut costs” would be; and it served as a liberal response to the overemphasis on the budget in the policy discussion about health care costs.
The difficulty is, “bending the curve” is a flawed way to think about the policy challenge. By focusing on the future, it diverts attention from cost controls that would have more immediate effects. In the middle of the worst economic crisis since the 1930s, that may be a good idea for budgeting. It is not such a good idea for health care spending.
The Metaphor’s Assumptions: A Flawed Guide To Policy
The assumption behind the metaphor is that there is a functional relationship of costs over time; presumably not caused by time but by some set of independent variables (technology, insurance, or whatever). So we can “bend the curve” at time X (say, in health care reform legislation in 2010) by changing those variables, with a predictable and desirable effect at time (X + Y).
This assumption has a major flaw: it downplays human agency. Policies do not simply play out and have predictable effects. People who object to the planned effects fight back. Health care costs at any time are the result of, among other things, efforts by people who earn their incomes from the system to extract money from it. If prices are lowered, providers may try to increase volume; if volume is constrained they may try to raise prices; if employers and insurers demand better prices the providers consolidate to increase their market power; if regulation is successful the providers claim the public is being denied quality care or campaign to create parallel markets where people can pay more for more “choice.” Whatever policy-makers do in Year One, the health care industry will seek to undo by Year Five or Year Ten. The metaphor of “bending the curve” ignores the fact that health care spending is a political/economic struggle. Either there is no function, or policy-makers are not the only ones who get to manipulate the terms of the function.
The flaw matters because the “bending the curve” metaphor directs attention to what its advocates would call “fundamental change,” and supports scorn for mere “short-term measures.” In the U.S. debate this was manifested especially in claims that reform had to reorganize delivery systems and the whole incentive structure of medical care, and in dismissal of factors that explain the differences between current spending in the United States and other countries. The major differences are prices and administrative costs, but in a typical report on “steps to address long-term spending growth,” ten of the best-known analysts in the United States started “from the conclusion that the standard short-term measures to address rising costs, like reducing prices, are not sufficient to succeed.”
This kind of perception is reinforced by an underlying belief that the dominant delivery system reform agenda – measures such as “integrated delivery systems, bundled payments, and more sophisticated comparative effectiveness analysis” are much more attractive than “crude” measures such as “across-the-board cuts in payments.” Even analysts who have long emphasized the need to adapt a system to have the same advantages as those in other countries can be caught up in the argument that much more fundamental changes are needed. Thus Tim Jost editorialized that a new Independent Payment Advisory Board created by the 2010 legislation was flawed because the “requirement that the IPAB submit annual proposals will encourage recommendations for short-term payment fixes rather than long-term changes that might in fact bend the cost curve.”
The evident problem with this focus on long-term measures is that nobody knows how to implement the various theories being proposed, such as how to create high-value “accountable care organizations.” On the one hand, the long-term focus makes it easier to advocate measures that we do not know how to do now: it is easier to advocate half-baked ideas if there is still time for some baking. On the other hand, as a taxpayer and citizen I would prefer not to rely, for cost control, on notions such as that, “these changes could spark a productivity revolution in health care that would make it much more affordable and simultaneously increase the quality of care.” The “could” is not reassuring, and the “productivity revolution” concept risks ignoring the challenge of capturing the benefits of increased productivity for the payers, rather than the providers. One of the reasons for addressing prices is to ensure that, for example, technological advances that make cataract surgery less expensive are reflected in lower prices, rather than simply higher earnings.
The de-emphasis of prices and administrative costs as “crude” concerns must be comforting to insurance company managers and medical providers. As an approach to long-term costs, however, it ignores a basic rule of mathematics: that the product of the operation of a rate of growth on a base can be altered by changing either the growth rate or the base. Hence long-term spending projections for Medicare were cut substantially by the sharp slowdown in Medicare spending in the late 1990s. A recent analysis in Health Affairs projects how shifting the level downward at any given time can have major effects on future costs; both reducing the level and reducing the growth rate are important.
Hence the “bending the curve” metaphor has two flaws as a guide to cost control. First, it suggests that there are measures that could be taken which would definitively shape future costs. This is at best questionable. Second, it directs attention away from measures that would reduce costs in the short term. This is particularly unwise since controlling costs in the short term is one of the better ways to influence future costs.
A Dangerous Metaphor, But Real Questions
The fact that we can graph costs leading up to the present does not mean that systems are on a mathematically predictable path. Future costs cannot be determined at a single point in time. They will depend on policies, responses, and unexpected events at many different times in the future: next year, in three years, in five, in eight, and so on. To a great extent, health care spending control must operate in the present tense, and controllers ought to be modest about the future.
Yet there are questions and policy choices that require judgment and evidence about results fairly far in the future. Although cost control is an endless battle, certain system features can normally favor one side or the other. For example, there are reasons to believe that systems that provide insurance to cover charges from providers tend to make it more difficult to control spending than systems that entitle people to access a government sponsored health service (Note 1). Similarly, there is strong evidence that all-payer price regulation is more effective than selective contracting if the goal is to reduce prices.
Each of these patterns has exceptions that prove the larger rule: that cost control requires continual effort. There have been times when spending grew more quickly in Sweden than in Germany, and times when it grew more quickly in Germany than in Sweden. Selective contracting controlled prices more successfully in the United States in the mid-1990s than it normally does. Still, it makes good sense to work to create institutions that provide better cost control tools in the future.
There are many reforms that might improve cost control in a given system in the future, and if we were only to focus on immediate effects we could miss useful options. Policy options such as increasing the number of primary care providers or installing better electronic medical records, could only save money, if they do so at all, in the long run. That is not a reason to reject them.
Yet it is a reason to be very cautious about such ideas, and to look for compelling evidence, preferably based on experience rather than deduction. The fact that something requires deep systemic change does not make it a good idea. Given the uncertainties about long-term approaches, it is even more important to maximize success in the short run: that is, adopt measures that somewhat restrict costs with acceptable consequences for other values.
I do not mean to suggest that excessive focus on the future is the only reason why policy-makers hesitate to address costs more quickly. The many parts of the medical industry are powerful and resist restrictions on their earnings. If the 2010 health care reform laws had included more immediate cost controls, they probably would not have passed. Yet, precisely because of such difficulties, it is important to the maximize political will for cost control and an understanding of what will work best.
From this perspective, the merits of framing the cost control problem as how to “bend the curve” are outweighed by the risks. Framing the problem this way risks believing that policy has more control over the future than it possibly can; risks ignoring the extent to which cost control is a political struggle rather than a technocratic challenge; and directs attention to situations about which we know and can do less (the future) rather than about which we know and can do more (the present). And, while this need not be the case, and I believe was not the intent of the idea’s originators, as used in the U.S. debate the focus on “bending the curve” has favored speculative ideas over measures with which there is more experience.
Source: Health Affairs